New Findings from the Team of Academician Jia Weiping at the Institute for Active Health Strategy and Development, Shanghai Jiao Tong University: This Dietary Fiber in Food May Help with Weight Loss 2024-02-29
A new solution for obesity treatment has emerged. On February 26th, Nature Metabolism, an authoritative journal in the field of metabolism, published research findings from the Endocrinology and Metabolism Department of the Sixth People's Hospital affiliated with Shanghai Jiao Tong University and the Shanghai Key Laboratory of Diabetes. The study discovered that resistant starch and a balanced diet can alleviate obesity by regulating the gut microbiome.
An expert commentary titled "Resisting Weight Gain with Prebiotic Fiber" accompanied the publication, highlighting the study's revelation of the clear efficacy of microbial group targeting treatment for metabolic diseases. It suggests that optimized microbial treatment methods are the hope for the future.
Obesity, a chronic disease, has become a global public health crisis. Exploring effective measures to prevent obesity and control weight is significant for promoting the health level of the entire population.
Gut microbiome disorder is one of the initiating factors of obesity. Dietary intervention to adjust the gut microecology presents a promising strategy for obesity treatment. Resistant starch is a type of dietary fiber naturally found in foods, mainly sourced from green bananas, potatoes, and rice that have been cooked and then cooled, whole grains, and legumes. It is not easily broken down and absorbed by digestive enzymes in the small intestine but enters the large intestine to be fermented by microbes, holding the potential to regulate the gut microbiome.
Therefore, Professor Jia Weiping and Professor Li Huating's team from the Endocrinology and Metabolism Department of the Sixth People's Hospital affiliated with Shanghai Jiao Tong University Medical School, the Shanghai Key Laboratory of Diabetes, and the Institute for Active Health Strategy and Development at Shanghai Jiao Tong University conducted a series of studies on the dietary treatment of metabolic diseases with resistant starch.
The researchers initially carried out a randomized, controlled, crossover clinical trial on overweight and obese participants. Thirty-seven participants were randomly divided into two groups; one group first underwent an 8-week intervention with resistant starch (40g/day), and the other group received an 8-week intervention with an isocaloric control starch. After a 4-week washout period, the interventions were swapped, followed by another 8-week period of resistant starch and control starch intervention respectively.
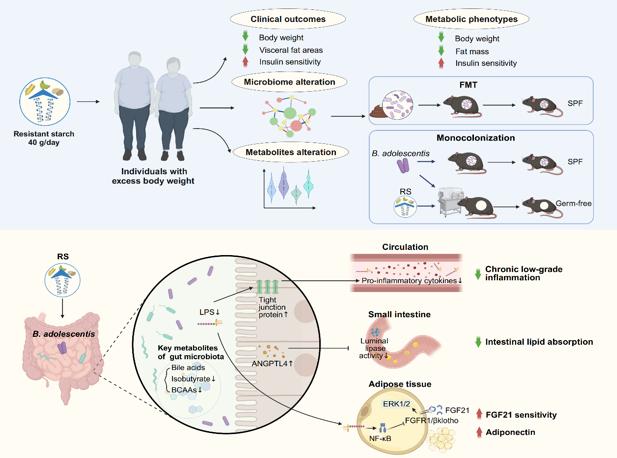
The results showed that after an 8-week intervention with resistant starch combined with a balanced diet (calculated total energy intake based on height and physical activity level, averaging 1600-1700 kcal/day, with 50–60% from carbohydrates, 25–30% from fats, and 15–20% from proteins), overweight and obese participants lost an average of 2.8kg. There was a significant reduction in visceral fat, and insulin sensitivity assessed by clamps improved significantly, whereas these effects were not observed during the control starch intervention period.
After the resistant starch intervention, participants showed significant improvements in systemic chronic inflammation levels, increased fecal lipid content, significant elevation in Angiopoietin-like protein 4 (ANGPTL4), and decreased levels of Fibroblast Growth Factor 21 (FGF21).
Through multi-omics exploration, the researchers found that resistant starch intervention significantly increased the abundance of Bifidobacterium adolescentis in the gut microbiome, key to the improvement in overweight and obesity by resistant starch.
Further human-mouse fecal microbiota transplantation and germ-free mouse single-bacterium intervention experiments revealed that the weight loss benefits of resistant starch depend on the gut microbiome. This effect is partially mediated by B. adolescentis, which can upregulate the production of ANGPTL4 in the small intestine. ANGPTL4 can inhibit the activity of intestinal lipase, thereby blocking the absorption of lipids from food. B. adolescentis can also restore the intestinal barrier damaged by obesity, reduce circulating inflammation and LPS, and inhibit the activation of TLR4/NF-κB in adipose tissue, enhancing tissue sensitivity to FGF21, thus combating obesity and insulin resistance.

Professor Jia Weiping (left) and her team
The team's previous research found that resistant starch intervention is a new treatment for metabolic dysfunction-associated fatty liver disease, with improvement effects independent of weight loss. Besides the increase in B. adolescentis, it was observed that resistant starch reduces the opportunistic pathogenic commensal Bacteroides stercoris, decreases the production of bacterially-derived branched-chain amino acids, alleviates liver fat accumulation and inflammation (Cell Metabolism, 2023).
This study, for the first time through a randomized, double-blind crossover clinical trial, proved in an overweight and obese population that resistant starch combined with a balanced diet might become a new strategy for treating obesity. It revealed its mechanism through reshaping the gut microbiome, with the key functional bacterium B. adolescentis increasing in abundance after the resistant starch intervention, alleviating obesity through mechanisms like improving the intestinal barrier function, reducing inflammation levels, and decreasing the absorption of dietary lipids.
The study's crossover design noted weight rebound during the washout period, which is one of the main challenges of long-term weight management. Thus, long-term intake of resistant starch combined with a balanced dietary habit to maintain gut homeostasis is crucial for weight control, integrating sustainable interventions into daily life as the optimal solution for obesity.
Resistant starch, naturally present in foods and also available as a dietary supplement, offers an effective, economical, and sustainable lifestyle intervention for the treatment of overweight and obesity. This study provides a new approach to developing microbiome-based weight loss interventions.
Professor Jia Weiping from the Sixth People's Hospital affiliated with Shanghai Jiao Tong University, Professor Li Huating, Professor Xu Aimin from the State Key Laboratory of Biomedical Technology at The University of Hong Kong, Professor Gianni Panagiotou from the Leibniz Institute for Natural Product Research and Infection Biology - Hans Knöll Institute, Germany, and Professor Liu Xinyu from the Dalian Institute of Chemical Physics, Chinese Academy of Sciences, are the co-corresponding authors of this paper. Professor Li Huating, PhD student Zhang Lei from Shanghai Jiao Tong University Medical School, Professor Li Jun from the Department of Infectious Diseases and Public Health at City University of Hong Kong, and Master's student Wu Qian from Shanghai Jiao Tong University Medical School are the co-first authors.
Additionally, Professor Ye Jianping from the Center for Metabolic Disease Research at Zhengzhou University, Professor Xu Guowang from the Dalian Institute of Chemical Physics, Chinese Academy of Sciences, and Professor Zhao Yueliang from the School of Public Health at Shanghai Jiao Tong University provided active support and methodological suggestions. The research was funded by the National Key R&D Program, the Major International (Regional) Joint Research Project of the National Natural Science Foundation of China, the Research Grants Council of Hong Kong, the European Union Horizon 2020 project, and the Young Researcher Project on Gut Microbiota by Convergence Pharmaceuticals, among other funds.
Translated from Wenhui Daily.





